TRANSGENDER HAIR TRANSPLANT
Confidence boost
Dr Bessam Farjo presents a life–changing hair transplant for a transgender patient
DR BESSAM FARJO
Dr Bessam Farjo co-founded The Farjo Hair Institute in 1993, which is also a research and education centre. He exclusively practices hair restoration surgery and medicine in Manchester and London. He is also co-founder of the British Association of Hair Restoration Surgery (BAHRS).
CONSULTATION
Samantha was a patient who presented with male pattern hair loss at our clinic. She had previously undergone surgery to transition from male to female and was happy with how she looked, but then her hair started to fall out. She was a female but with male hair loss, and she said that this was affecting her mental health. She wanted to be able to have long hair but the hair loss she was experiencing made her feel self-conscious. She felt her hairline was too masculine so came to us to see if there was anything we could do to help restore her hairline and make her feel more feminine.
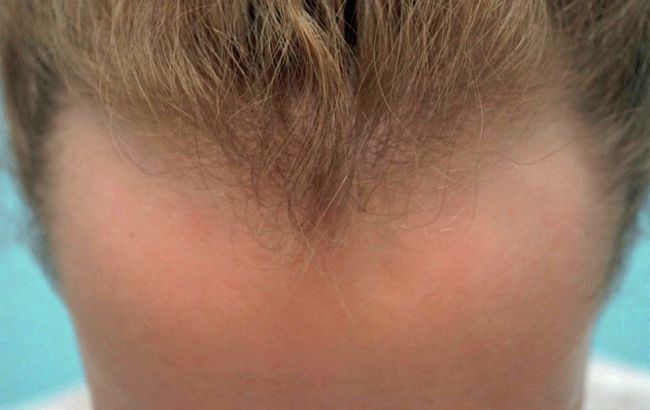
Before
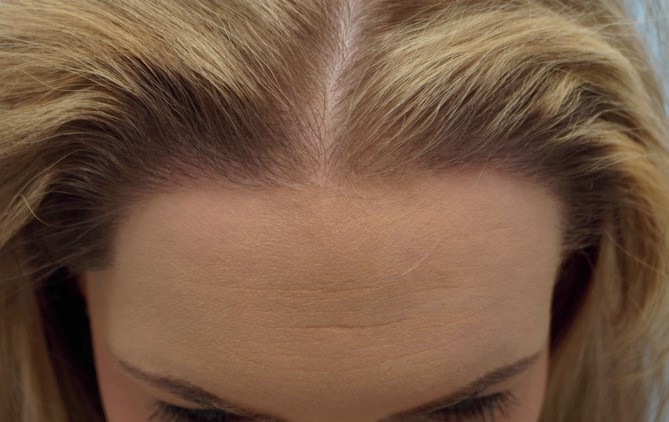
After 12 months

Before

After 12 months
Transgender patients are often good candidates for hair transplant procedures. Testosterone is converted in the body to dihydrotestosterone, AKA DHT, and DHT is a major culprit when it comes to pattern baldness. DHT will attach itself to a person’s hair receptor cells, which in turn reverses the process of hair growth and causes the follicle to shrink and disappear. However, transgender patients undergoing hormone therapy are given, among other things, estrogens and antiandrogens which can actually combat DHT. In the case of those who have already undergone gender reassignment surgery, the source of the vast majority of testosterone is removed. All of this means that hormone therapy or gender surgery can prevent a hairline from receding any further. However, any hair that was lost already can be replaced with a hair transplant in that area effectively and in a long-lasting fashion.
As you can see from Samantha’s before photos, there was no other option but surgery. She had mentioned she’d explored the use of laced wigs and cornrows, but both options were quite expensive long-term and had time and cost implications, and her frontal hairline was too high up. In the end, she decided that surgery would be a better longer-term investment. The choice was between hair transplant surgery and hairline advancement flap surgery. Both have pros and cons and we discussed this at length with Samantha. In the end, she opted for strip FUT (follicular unit transplant) hair transplant surgery to avoid a linear scar on her hairline, which would have occurred if she had gone with the flap-type surgery.
Additionally, there was still the possibility of further hair loss developing elsewhere on her scalp, so medications to maintain the hair were recommended. In Samantha’s case, finasteride and minoxidil.
Strip FUT is ideally suited to patients suffering from advanced hair loss who require large amounts of restoration and high graft numbers. Additionally, for both cisgender and transgender women, it allows them to have this done without having to shave long hair. The alternative is an FUE procedure (follicular unit excision) which is more popular with men and normally requires shaving the donor area. We discussed at length the type of desired female hairline that Samantha would like.
Accordingly, the number of hairs possible to implant was worked out. We did warn Samantha that a second procedure may be required to achieve the density she desired and that was comparable to the rest of her hair. As it happens, the one procedure turned out to be enough and she was thrilled with the results.
TREATMENT PLAN
While no two strip FUT procedures are ever exactly identical, they do follow the same essential steps from start to finish. Depending on the extent of the area to be treated and the number of grafts that need to be transferred, the procedure can take from 4 to 12 hours. Routinely we are able to transfer up to 4,500 grafts (up to 12,500 hairs) in one day.
Patients are given a mild sedative and local anaesthetic in both the donor and recipient areas. The discomfort felt for a few minutes when being given the anaesthetic (similar to what one feels when undergoing dental work) is the only sensation felt throughout the treatment. Once the anaesthetic has had its effect, the procedure begins by removing a thin strip of scalp containing healthy hair roots – genetically programmed to grow throughout the patient’s lifetime – with the aid of high magnification.
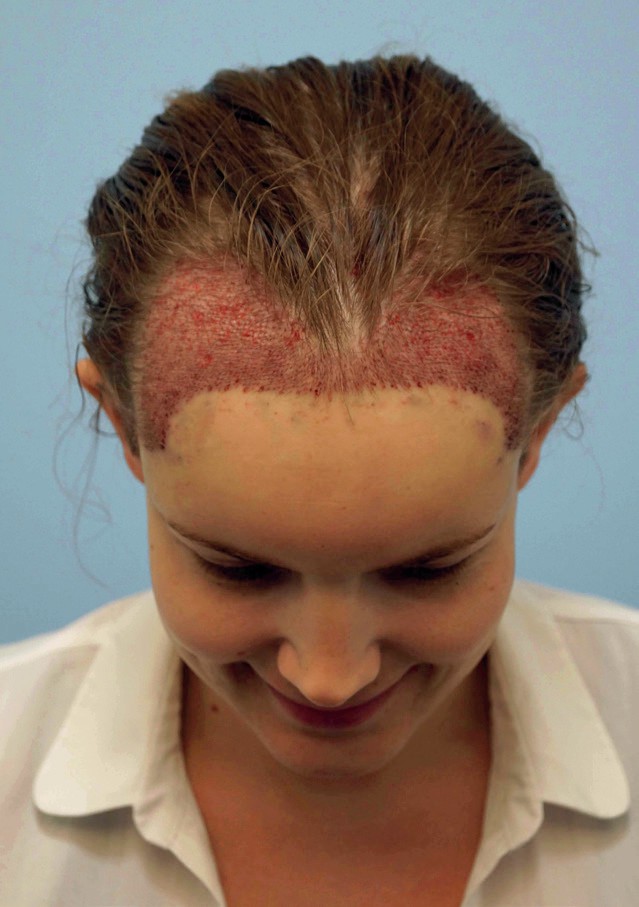
immedietely

After 12 months
Using stereoscopic dissecting microscopes, the strip is then divided into individual follicular unit grafts (each measuring approximately 1mm in width) – the use of microscopes means that about 30% more hair is harvested than with the use of older techniques. While this is happening, micro slits are made in the receiving area of the scalp using a variety of needles or tiny blades and, when ready, the follicular unit grafts are individually inserted. The grafts are blended in among the thinning or balding areas in such a way as to match all the natural growing characteristics of the original hair. We prefer to densely pack at a rate of 35-50 grafts, or 80-110 hairs, per square centimetre, per operation – in our experience, this represents the optimum number for a maximum hair survival rate of 85-90%. This means that one operation adds on average 25-30% of the original hair density.
The site from where the donor strip was sourced is closed using fine stitches or small surgical staples that are immediately covered by the surrounding hair. This normally heals to form a thin, vague and hard-to-detect scar among the permanent hair. With a few exceptions, we usually use what is known as trichophytic closure – this involves trimming one edge of the cut prior to closure, so that when the opposing edge of the cut is joined to the trimmed edge, hairs from the trimmed edge grow through the resulting scar, effectively camouflaging its appearance further. The entire procedure is very clean and, when complete, no bandages or dressings are required. With the expertise we offer at every stage of the procedure, we can produce results where the transplanted hairs are virtually indistinguishable from the original ones – even under the closest scrutiny.

Within half an hour of the treatment ending, the patient can be on their way home, although we strongly recommend they do not drive, so we advise that they make arrangements to get home by taxi or public transport or get picked up by a friend or family member.
RESULTS
Samantha was thrilled with the results. This was in part down to discussing her expectations in detail prior to the operation. She tolerated the process very well, as do the majority of patients. The post-operative routine is only needed for the first week or two in terms of very careful washing and no touching the head, as well as avoiding exerting exercise for that period. After that, patients can treat the new hairs the same as the rest. Afterwards and long-term, patients can expect the hairs to behave in a similar manner to where they come from at the back and the sides of the head. After her surgery, Samantha said: “Before my operation, I was distressed and depressed. Mentally, when I had the hair transplant, I had the freedom to walk down the street with confidence, knowing that it was my own hair. It was such a lovely feeling that I can’t really explain”.