OCULOPLASTIC SURGERY
Modern eyes
Cosmetic eye surgery has been refined into a delicate art that gives better results with less downtime, say oculoplastic surgeons Rachna Murthy and Jonathan Roos
RACHNA MURTHY
Rachna Murthy BSc(Hons) MBBS FRCOphth completed her post-residency fellowship training at Moorfields Eye Hospital, the Craniofacial Unit at Chelsea & Westminster Hospital and the Royal Victorian Eye and Ear Hospital in Melbourne, Australia. She has provided quaternary oculoplastic care for the East of England and sits on the board of Royal Society of Medicine’s Opthalmology section. Follow her on Instagram: @drrachna_murthy.
JONATHAN ROOS
Jonathan Roos PhD FRCOphth co-founded FaceRestoration clinic in London with Rachna Murthy. He is a Cambridge, Harvard and Moorfields-trained academic and consultant eye surgeon specialising in periocular cancer, orbital pathology and cosmetic lid surgery. He has published in excess of 50 papers and contributes book chapters on topics including aesthetic management of thyroid eye disease and nasolacrimal duct obstructions. Follow him on Instagram: @drjonathanroos.
One of the exciting things about being a doctor and surgeon is the constant innovation and change – aesthetic plastic surgery today would be unrecognisable to a surgeon from 30 years ago. Though we still use cold steel, our techniques are enhanced by lasers, bacterial toxins and injectable sugars to mention but a few. But perhaps the most important change is the emerging trend of conservative surgery to create a natural look. People now want to look younger, fresher and happier, not “done”.
This is particularly so on the face. As oculoplastic surgeons we know that the periocular area – the eyelids and brows – does not just protect one of the most important organs of the body, but is used to communicate non-verbally, particularly via our emotions. Even very subtle changes in the eyelids can alter how other people perceive us; ageing or inappropriate surgery can create a sad, tired or angry expression.
So, the job of an oculoplastic surgeon is to respect and restore the anatomy while enhancing desirable features without altering the identity of the patient. The patient looking younger and fresher but still like themselves is the best possible aesthetic outcome.
NEW AND IMPROVED
Ageing is first noticed in the eyelid area. Firstly, because it is where we focus when we speak to people and secondly, because it is an unusual area of the body. It is constantly moving with expressions and blinking, and its skin is among the thinnest on the body. It is also constantly exposed to the elements – sun, wind and pollutants – and so the skin begins losing collagen and hydration as early as our 20s. With loss of plumpness from receding underlying bone and muscle movements we develop fine lines and wrinkles. The orbital septum, a thin, cellophane-like sheet that holds our orbital fat, cushioning our eyes back, weakens, allowing fat to prolapse forwards and down into the lower eyelid, creating dark circles and shadows. The muscles become loose, as do the ligaments and tendons supporting the tissues.1
It is an improved understanding of this process of ageing – and the loss of tension leading to a loss of tensegrity (integrity through tension)² – that has allowed novel and less traumatic treatments to develop for our aesthetic patients. Modern surgery and non-surgical interventions aim to reposition and tighten structures that have moved or stretched, while avoiding those that have not been disturbed.
DARK CIRCLES AND TEAR TROUGHS
One example of this is how we manage tear troughs and dark circles. While previously we would have performed large, aggressive face lifts (risking injury to the facial nerve that controls all facial movement), we now have a number of options. We understand that much of dark circles has to do with shadowing from light coming from above and that some subtle placement of filler can last for years and offer patients immediate results with little downtime.3 These fillers have to be applied meticulously, respecting the anatomical change with tiny amounts in the tear trough on the bone where bone changes have occurred, lifting from the lateral cheek with filler and replacing small amounts of volume in the SOOF (suborbicularis oculi fat), which descends and loses volume. This avoids unnatural results and the need for reversal that we often see in our practice as complications support for aesthetic practitioners. ⁴
Surgery is now smaller and involves either fat repositioning or draping or a midface-only lift which is safer than a traditional face lift. We also no longer just cut away fat, as we understand that with age fat can atrophy and leave people skeletonised in appearance. We therefore prefer to preserve and reposition to restore. Another advancement is that surgeons have learnt to pre-empt problems by improving tension during the healing process. Complications of lid in-turning and out-turning can occur but are now prevented by the placing of reinforcing sutures (a canthopexy) at the time of surgery. Their aim is not to change the appearance but to support the lid during the healing process.
FESTOONS AND MALAR OEDEMA
For every step forwards however, we can have two steps back, and so it has been with tear trough filler. We are frequently referred patients who have had injudicious or excessive filler to the periocular area. After reversal with injection of a filler-dissolving enzyme, the skin can be left looking lax and wrinkled. For this, a surgical intervention is the only option. Laser procedures or other non-surgical skin tightening is unpredictable and can result in lower lid skin that is too tight – preventing eyelid closure and blinking, and in turning causing dry eye and discomfort and even an unsightly out-turned lower lid called ectropion. So, it is important to counsel patients adequately who insist they do not want surgery, especially if nonsurgical interventions are not appropriate for the degree of change in the anatomy.
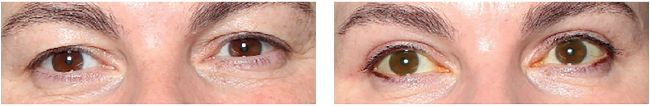
Blepharoplasty. Left: before, Right: after
DERMATOCHALASIS
This refers to excess upper lid skin and hooding and the main intervention remains the blepharoplasty. It is still the most common procedure we perform and it has the biggest impact on the face. However, even here things have changed. Previously the domain of general plastic surgeons, there is a growing understanding among patients and surgeons alike that the eyelids are a specialised area requiring specialist skills. Eye examination for underlying pathology is key to a safe procedure, lest one trigger scarring disorders, injure small muscles that affect eyeball movement or remove a lacrimal gland. Dryness, double vision or even blindness can then result.
Not all innovations have been helpful – introduction of the plasma pen to cause focal scarring in a grid and thus obliterate excess tissue can be unpredictable. We have operated on patients in whom there has been considerable scarring which results in additional bleeding during surgery and which, with lost tissue planes, is slower and more challenging.
Previously, upper-lid blepharoplasty would involve removal of skin, muscle and fat. This can result in a sunken and hollow appearance with ageing and when it occurs more medially is termed an “A-frame” deformity. To avoid this our surgery is now much more minimalist – often skin alone is removed rather than muscle, fat is sculpted rather than excised and the septum strengthened rather than weakened. Where there is a deformity, we can also drape orbital fat medially and laterally, though usually this is not necessary. We are also careful to gently reposition the lacrimal gland which can fall forward and out of the orbital socket with age. A small brassiere suture to the capsule will anchor it inside the rim.
There have been some other treatment developments which can be combined or used instead of surgery in the short term. For example, botulinum toxin will increase the brow height, lifting the skin of the lid and making it less hooded. But very high brows will create a surprised or confused look. Filler to the temples and zygoma can also affect the position of the lateral corner of the eye and lid hooding and may be beneficial alone or in combination with surgery for some patients.
PTOSIS
This refers to a dropped rather than hooded lid, though the two can occur at the same time as they are usually both age-related conditions. Here too there have been developments, starting with the development of a posterior and anterior approach 40 years ago but now with a change in the anaesthetic. Rather than sedation or general anaesthetic, ptosis surgery is now performed with the patient fully awake and with only minimal local anaesthetic. This is to enable movement of the eyes and lid during surgery so that the height of the lid can be set correctly and symmetrically. This allows for less downtime, less swelling and bruising, shorter patient stays and better judgment of the aesthetics. So, aesthetic surgical advances are not limited to just the surgeon but to the entire perioperative care.
Teaching has also improved – there are some droopy lids that can suggest very serious underling medical problems. Every medical student will now know how to recognise these due to improved online and in-person teaching. We contribute to this safety aspect of surgery by running our own surgical training course for plastic surgeons in Cambridge.⁵
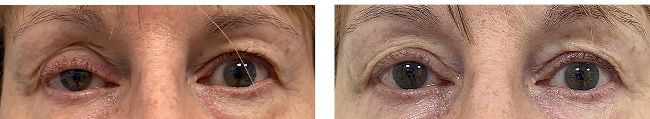
Right upper eyelid ptosis surgery without blepharoplasty. Left: before, Right: after
FULL CIRCLE
Some surgeons are happy to perform the same operations and treatment algorithms they were taught during their own training, sometimes decades ago. But the best surgeons adapt and develop new skills. One thing that we believe we have done well at FaceRestoration is to embrace new technology. We invested early on in 3D photographic imaging to be able to demonstrate objective effects of our treatments to patients. It is remarkable how pleased patients will be after a treatment and then grow used to their new appearance. Being anchored in time with good photography helps remind patients where their journey started and probably helps all of us avoid doing too much.
Despite leaving the NHS, we have both remained engaged in research to ensure that we are delivering the best and latest treatments for our patients. One such result has been the Scars-less approach to surgery, which is our trademarked means by which we are able to perform surgery that will scar less, as well as the patent-pending perioperative and daily use professional antimicrobial spray Purifeyes. This is an exciting development, because though hypochlorous has potent anti-microbial and anti-viral properties, as a powerful molecule it is also unstable. Working together with a medical manufacturer we were able to create a format that can be used straight on the eyelids and eyes, which does not sting and remains stable. We now use it when we remove sutures and to help reduce inflammation after surgery, as well as aftercare for all our patients undergoing injectable treatments with hyaluronic acid filler.

We have also kept up to date with new technology. New forms of hyaluronic acid fillers are able to achieve long-lasting lifts which older versions could not. We are able to achieve much of our facial rejuvenation without surgery in a clinic appointment. Patients get a fresher, rejuvenated look with an improved periocular appearance, all without local anaesthetic, bruising or any downtime.
Especially now thanks to covid-19, we are seeing changes in the periocular and facial aesthetic sector – it is no longer the preserve of women. Encased in their masks for a year, and with many out of work and feeling low, men too have found that they can feel better when they look five to 10 years younger. For some men, looking in the mirror can be considered a bit “unmanly”, but no one has been able to escape the picture of themselves emanating from zoom screens.
REFERENCES
1. Facial Topography: Clinical Anatomy of the Face by Joel E Pesa, Rod J Rohrich. Quality Medical Publishing, Inc., St. Louis, Mo: 2012.
2. Buckminster Fuller (1895-1983) an American architect, systems theorist, author, designer, inventor and futurist used the word ‘tensegrity’ to describe a structure whose form relies both on compression and tension.
3. Murthy R, Roos JCP, Goldberg RA. Periocular hyaluronic acid fillers: applications, implications, complications. Curr Opin Ophthalmol. 2019 Sep,30 (5):395 – 400.
4. Murthy R, Roos JCP, Goldberg RA. Periocular hyaluronic acid fillers: applications, implications, complications. Curr Opin Ophthalmol. 2019 Sep,30 (5):395 – 400.
5. www.aesthetics-course.com.