MANAGING SEVERE INFLAMMATORY ACNE USING MEDICALLY CERTIFIED LED PHOTOTHERAPHY
Tara Morgan describes the use of medical grade LED phototherapy within her aesthetic practice to manage severe inflammatory acne in a patient who was unable to tolerate conventional systemic treatments
PATIENT OVERVIEW
Patient: Stella Chai
Age: 27 Skin concern: Cystic acne
Treatment: LED phototherapy (Dermalux Tri-Wave MD)
Sessions: 16
Timeline: Three to four months
TARA MORGAN
Tara is a registered nurse and midwife having worked in the NHS for over 15 years. Tara specialised in surgical nursing, working in areas such as Urology, ENT, Breast and general surgical settings. After having her own children, Tara pursued a different career pathway into aesthetics and has been working as an aesthetic practitioner since 2019.
Cystic acne sits at the severe end of the acne spectrum. Lesions form deep beneath the skin, are painful and carry a substantially higher risk of scarring than comedonal or mild inflammatory presentations.1 While acne affects up to 80% of individuals between 11 and 30 years of age, cystic cases are far less common and considerably more challenging to manage. The psychological burden is also disproportionate, particularly when facial involvement is extensive.3 Management is usually medically led. Topical therapies, oral antibiotics and isotretinoin remain the standard option.1 But these approaches don’t suit everyone and can come with some unwanted side effects.
Side effects, contraindications and treatment fatigue limit tolerance, leaving some patients with few acceptable options. Many begin looking for non-systemic alternatives at this point.
PATIENT PRESENTATION AND PRIOR TREATMENT HISTORY
Tara Morgan explains a significant case she treated with LED phototherapy. At presentation her patient’s skin showed marked erythema, widespread inflammation and multiple deep cystic lesions beneath the surface. Lesions were painful, persistent and without visible heads. The pattern was one of continuous activity rather than a discrete flare and the face was primarily affected. The condition had been present since adolescence.
The emotional impact was obvious. The patient described reduced confidence and ongoing distress.
“You could see how much it was affecting her, not just physically but emotionally,” noted Tara this is not unusual. Severe acne is consistently associated with greater psychological distress than milder forms.3
The patient had been managed through GP and dermatology services over seven months. Treatment included topical and oral therapies in line with clinical guidance.1 None provided sustained benefit. Topical agents caused pronounced dryness and cracking, indicating a compromised barrier. Oral acne medications were poorly tolerated due to the patient’s ulcerative colitis. Options had narrowed considerably.
This pattern of brief improvement followed by relapse once treatment stops is common and frustrating. Given this background, further escalation within the aesthetic setting was neither appropriate nor desirable.
TREATMENT RATIONALE AND PROTOCOL
LED phototherapy was the most appropriate option available in clinic. It addressed inflammation without adding irritation or systemic burden. When applied correctly, energy-based devices have been shown to support acne management with a favourable safety profile.2
Treatment was delivered using the Dermalux Tri-Wave MD, a Class IIa medical-grade LED phototherapy system capable of delivering up to 240 J/cm² per session.
The early focus was deliberately conservative. Rather than targeting surface bacteria from the outset, the priority was calming inflammation and supporting recovery in the deeper layers of the skin. Near-infrared wavelengths at 830 nm were used during the initial phase. These penetrate the dermis and support healing processes associated with inflammation control.2
“The first aim was simply to settle the skin,” explains Tara. “Every time one area started to improve, another cyst would form underneath. Until that deeper inflammation was addressed, nothing else was going to work.”
This staged approach reflects an understanding that surface-level bacterial treatment is ineffective when deeper inflammatory processes remain active. Sessions using the LED phototherapy system were carried out twice weekly for the first two months, with each treatment lasting 20 minutes. As visible inflammation reduced and the skin stabilised, blue light wavelengths at 415 nm were introduced to support bacterial reduction.2 Treatment frequency was gradually reduced, first to weekly, later to once every 10 to 14 days.
CLINICAL RESPONSE
Changes were seen earlier than expected. Within two to three weeks, erythema had reduced and the number of active cysts had fallen.
“After about two weeks, her skin had gone from spotty, red and scabby to still red but without any active spots. It had calmed down considerably,” Tara observed.
By around six weeks, breakouts were approximately halved. The underlying pain and burning sensation had resolved. Texture improved and the skin appeared calmer overall. Given the severity of the initial presentation, described as “probably one of the worst cases I’ve seen of cystic acne”, the response was notable.
The intensive in-clinic phase consisted of approximately sixteen sessions over three to four months.
MAINTENANCE AND HOME-BASED TREATMENT
Once the intensive phase was complete, the patient transitioned to a portable Class IIa medical-grade LED device for home use (Flex MD, delivering up to 40 J/cm²). This allowed ongoing treatment at lower energy levels, applied more frequently to maintain stability.
“The machine I have in clinic is medically certified to treat moderate and severe acne and offers optimal dosing of light which can be easily adjusted for every case which is why we see faster and predictable results” Tara explains. “The one she uses at home is not as strong, so she needs to use it at least five days a week to maintain results.” This difference matters. Lower-output devices require more frequent use to achieve comparable outcomes.2 For practitioners managing complex acne presentations, understanding device capability is essential.
“Many consumer-grade devices deliver substantially lower energy levels and would not have achieved the same results in the same timeframe as the medical grade device.” Tara adds “Plus there are also many other parameters which need to be considered to ensure that biological processes are being triggered.”
PATIENT EXPERIENCE AND SCOPE CONSIDERATIONS
Managing expectations was important. Patients who have tried multiple treatments are often sceptical.
“It seems almost too easy sometimes,” notes Tara. “Patients often think they have to treat acne with aggressive medications. There is always that hesitation to keep throwing money at something when they cannot be guaranteed the outcome.”
A clear explanation of how the LED works, why inflammation was addressed first and what realistic timelines looked like, helped build trust and adherence.
It is also important to recognise the limits of aesthetic practice. LED phototherapy was offered after medical options had been explored. Referral pathways to dermatology remained in place. No attempt was made to investigate systemic or hormonal contributors. Adjunctive care focused on barrier-supportive, medical-grade skincare only.
Appropriate patient selection was critical in this case. The patient had been extensively managed through medical channels and was seeking a non-systemic alternative when conventional treatments had proven either ineffective or intolerable. This made her well-suited for LED phototherapy within an aesthetic practice setting.
As treatment progressed and the patient’s skin stabilised, Tara observed improved confidence and engagement with the treatment process. The patient reported feeling more comfortable with her skin and more positive about ongoing management, reflecting the impact that visible clinical improvement can have on patient satisfaction.
CONCLUSION
For this patient, medical-grade LED phototherapy provided a workable and well-tolerated route forward when other options had failed. Several factors contributed to success: appropriate patient selection, the use of a medical-grade system capable of delivering clinically relevant energy levels, staged wavelength selection that addressed inflammation before bacterial activity, and careful expectation setting.
Within aesthetic practice, medical-grade LED phototherapy offers a valuable noninvasive option for selected patients with severe inflammatory acne, particularly where tolerance of systemic treatment is limited.
REFERENCES
1. Zaenglein, A.L., Pathy, A.L., Schlosser, B.J. et al. (2016) ‘Guidelines of care for the management of acne vulgaris’, Journal of the American Academy of Dermatology, 74(5), pp. 945–973.
2. Nestor, M.S., Swenson, N. and Macri, A. (2016) ‘Physical modalities (devices) in the management of acne’, Dermatologic Clinics, 34(2), pp. 215–223.3. https://www.ucl.ac.uk/population-health-sciences/intune-uknational-menopause-education-and-supportprogramme
2. Tan, J.K. and Bhate, K. (2015) ‘A global perspective on the epidemiology of acne’, British Journal of Dermatology, 172(S1), pp. 3–12.
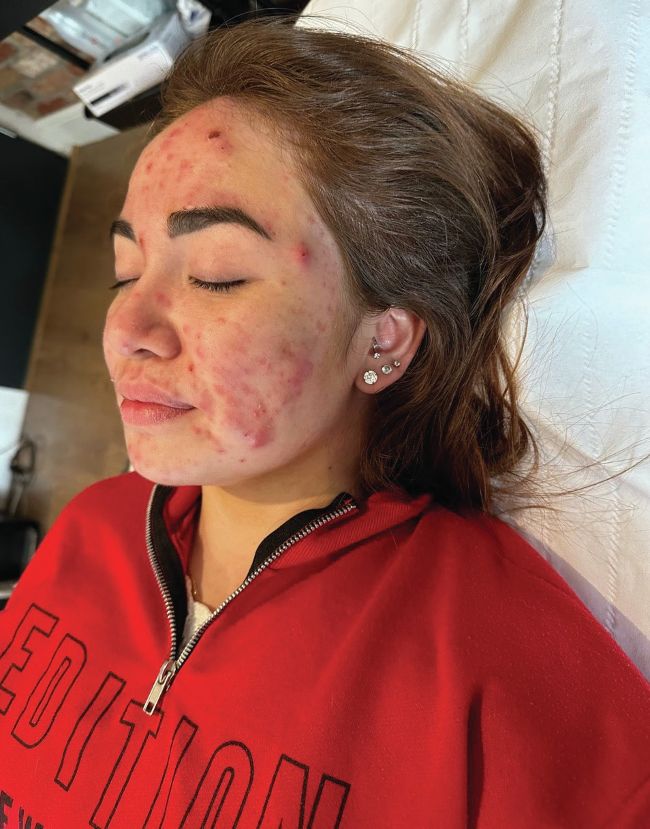
Before
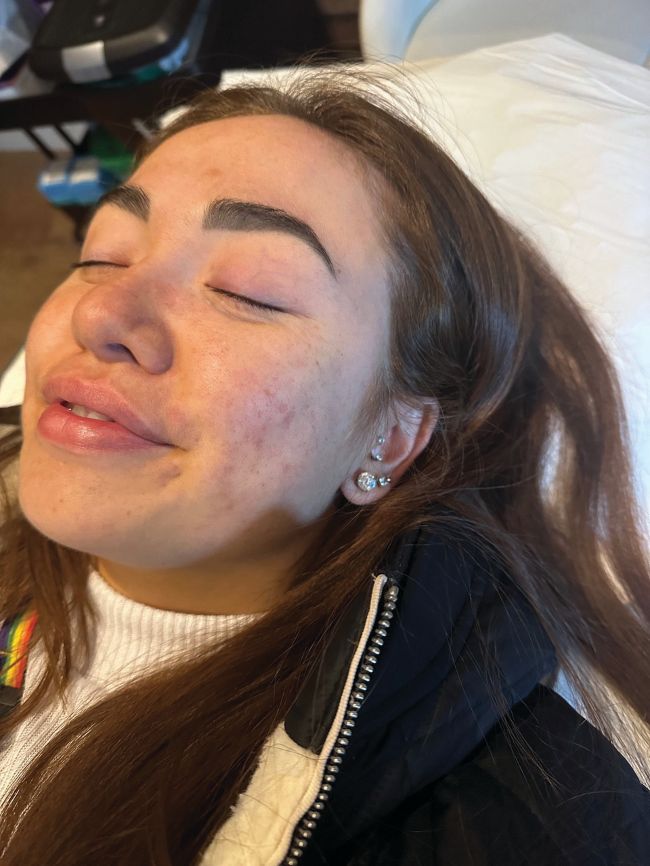
After