CLINICAL
Autologous medicine
Dr Paul Charlson considers applications and methods for PRP, PRF and stem cells
DR PAUL CHARLSON
Dr Paul Charlson is the director of Skinqure (Yorkshire) and Intoskin (London) Clinics and the medical director of Continental Skin Clinic (London). He is the past president of BCAM and JCCP board member. Dr Charlson has worked in aesthetics for 24 years and uses a range of autologous products, including T-Lab.
Harvey Barrett is head of business development for Hawksley and Sons who distribute T-Lab autologous products in the UK.
SKIN
Between every seven and 10 years, all the cells in our body will have been replaced by new ones. This phenomenon is called cell regeneration. From biological research into cell regeneration, the field of regenerative medicine has emerged, which is also known as tissue engineering or autologous medicine.
The principle of regenerative medicine is that we use cells from the patient’s own body, to accelerate the body’s natural healing pathways. Most people in our industry will be familiar with autologous medicine because of platelet-rich plasma (PRP or vampire facelift) treatments, where some of its basic principles were pioneered in the 1920s.
Technological advancements are leading to excellent outcomes for patients, without the need for expensive capital equipment.
Important autologous treatments are PRP and platelet-rich fibrin (PRF) obtained from the patient’s blood, and mesenchymal stem cells (MSC) obtained from skin, fat, placenta and bone marrow.
BLOOD
Blood contains platelets. Platelets are a source of growth factors. When platelets are concentrated in methods such as PRP and PRF, it also concentrates growth factors.1 Platelets are vital for wound healing and contain mitochondria, lysosomes, dense granules, and alpha granules (similar to exosomes).2The alpha granules contain a variety of proteins such as growth factors, adhesion molecules, cytokines and other products. When activated, they are essential for modulating inflammation and tissue repair, including collagen formation.
This is the basis of exosome treatment in regenerative medicine. Commercial exosome treatments in the UK are nonhuman, except when autologous (the patient’s own).
The advantage of autologous treatments is that they are derived from the patient, so they are biocompatible and generally free from the risk of contamination or adverse allergic reactions. No direct comparative studies have been performed between non-autologous and autologous treatments such as exosomes. Logically the most biocompatible products are likely to be the most effective.
SKIN
The skin is a complex organ that contains many different types of cells and compounds. Epithelial cells make up most of the skin and are the first protective barrier. Beneath epithelial cells lies the hypodermis, which is a mesh of fibroblasts that support a framework of collagen, hyaluronic acid, and elastin. The secretions from fibroblasts work like a scaffold that enables new blood vessels and the growth of new epithelial cells.
FAT
Adipose tissue is a network of adipose cells and pre-adipocyte progenitor cells, small blood vessels and pericytes, and then mesenchymal stem cells. All of this is held together by a spiderweb-like extracellular matrix, holding the fat together. Mesenchymal stem cells are some of the most flexible cells in our body and will differentiate into whatever type of useful cell our body needs to heal itself.3
EXTRACTION OF PRODUCTS FOR REGENERATIVE MEDICINE
Centrifuges
The problem to be solved for an autologous medicine product is how we separate everything useful to our body from the remaining unessential or harmful cells. This can be done either chemically or mechanically.
Centrifuges are a cheap and easy way to separate blood into the various products required such as PRP and PRF.
PRP, for instance, isolates and harvests platelets mechanically. By spinning whole blood in a centrifuge, the heaviest cells (red blood cells) are pushed to the bottom. Leucocytes (white blood cells) sit above the red blood cells. At the top, the lightest cells (platelets) rise and float in the plasma. However, if you spin too fast or for too long, platelets will get crushed, stopping them from activating and reducing how many total platelets are recovered from the blood. If centrifuged too slowly or for not enough time, the PRP will be less pure and contain red and white blood cells. Centrifuges separate particles by their weight; they are essential tools for anybody practising regenerative medicine and are relatively inexpensive. Amachine with a swing-out rotor and adjustable speed parameters is best. This is because it gives you flexibility to perform many types of regenerative medicine procedures, and the recovery rates for all treatments are better. Areview article on PRP suggested that a double spin method producing 1-1.5 million/ul is adequate for soft tissue and platelet activation is unnecessary.4 Another study confirmed the double spin method being preferable.5
PRF differs from PRP in the methods of extraction from the blood. PRP is extracted from blood tubes that contain anticoagulants and PRF tubes do not contain anticoagulants. The spin rates for PRF are generally slower. One disadvantage of PRP is that the use of anti-coagulant leads to a potential effect on growth factor release because it is linked to the clotting mechanism.6 Second, the release of growth factors is rapid and short-lived in PRP and this may limit its effect.7 PRF requires a shorter centrifugation. It produces a fibrin matrix entrapping platelets and leucocytes within it. A slow release of growth factors compared with PRP occurs.8 There are various ways to prepare PRF but liquid PRF is useful as the distribution of cells within it appears uniform.9 PRF provides a controlled release system for growth factors.10 Another showed better results with PRF than PRP in atrophic acne scars.11
Microlysers
Another essential tool for performing regenerative medicine treatments is a device that can break down cells and tissues used in the extraction of stem cells.
When we take tissues like skin and fat from the body, using, for example, a punch excision, we need to break the tissue down before it can be injected back into the host.
This is because tissue is bound together in matrices, containing both the useful and useless cells for a regenerative medicine treatment. Unfortunately, centrifuges alone cannot separate the strong extracellular matrices without significantly undermining the viability of these cells. This is the basis of stem cell technology.
An excellent solution is a medical device called a microlyser by T-Labs, which incorporates hundreds or thousands of honeycomb-shaped blades. The devices come in several sizes for the blades, from 41um (designed to filter out platelets) to 2400um (for initially breaking down the extracellular matrix in adipose tissue).

This simple-looking device avoids previous problems, like blockage and the quality of cutting. In the picture below, you will see that, under the microscope, the other devices have more simple meshes. This means that when tissue passes through them, it is not adequately dissected and is prone to getting trapped in the mesh, blocking the device.
Seher Yaylaci’s recent study proved the effectiveness of the new T-Lab microlyser, by analysing the viability of stem cells processed using one of T-Labs’ microlysers. Seher did this using flow cytometry, staining, and immunofluorescence methods after 14 days of culturing the adipose-derived stem cells. The results showed thriving and viable colonies of stem cells, fibroblasts and skin cells.
Use of MSC in aesthetics
MSC has been used in aesthetic medicine for some time. Extraction of the tissue and product preparation varies, making comparative research difficult. Most work has been done on adipose-derived stem cells (ADSC). A review article cites that they have been shown to accelerate wound healing, reduce scars, encourage hair regrowth and regenerate the skin, as well as improving fat graft survival.12 Another noted a significant improvement in hair density after three monthly injections of ADSC.6
Use of PRP and PRF in aesthetics
PRP and PRF can be grouped for therapeutic purposes. There appears to be some advantages to PRF outlined previously. One group performed a comprehensive review of PRP and concluded that it is useful in a variety of dermatological diseases such as plaque psoriasis, lichen sclerosis, alopecia and pigment disorders, as well as skin regeneration, stretch marks and wound healing.13
There are fewer studies for PRF, but all have been used in similar ways to PRP. A few comparative studies have shown that PRF has better results.
Delivery of the autologous product
The preferred method is injection, using a fine needle into the dermis or hypodermis. I could find no papers comparing results, but most papers seem to show that the injections are intradermal. The calibre of the needle appears to have no effect.14 Another found that pain was less with a 32g needle than 27-30g and pain was less at 0.9mm than 1.2 mm depth.15 Gordon Sasaki found that using 1mm microneedling and massage the optimal massage time was 5-20 minutes.16 Metin Görgü at al found a dose of 0.03ml compared with 0.01ml increased spread of PRP.17
CONCLUSIONS
PRP, PRF and stem cell treatments work. They have potentially multiple applications in aesthetic medicine and dermatology. They are safe and cheap to prepare. There needs to be more research into which treatments are most beneficial. Also, there needs to be standardised protocols to determine how products are prepared as we know that preparation is important. Similar methods of delivery may have a bearing on the outcome. Stem cells differ from PRF/PRP as they are undifferentiated immature cells but all methods act to repair tissue.
I could find no studies comparing stem cell treatments with either PRP or PRF or the method of administration. However, injected treatments appear favoured to smearing the products on the skin with assisted penetration via microneedling or TIXEL. Probably, the needling effects are also beneficial in all treatment modalities. The future of this field of medicine is bright and only likely to expand over time.
CASE STUDIES
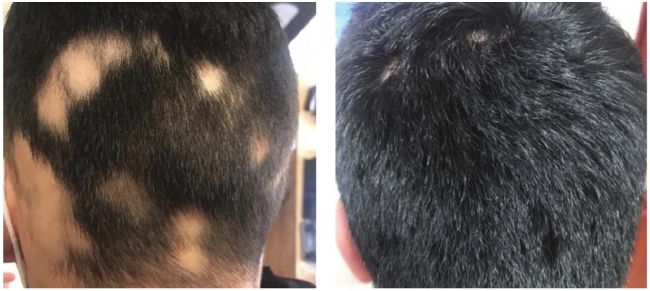
Case study one (before and after) This alopecia areata patient is aged 19. After having a very stressful first year at university, the stress had resulted in acute hair loss which had not grown back over the summer holidays. After three sessions of PRP, placed two weeks apart, a year on, he is much happier, and his alopecia has disappeared.
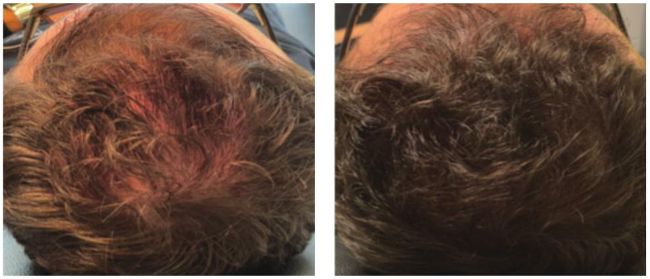
Case study two (before and after) While having a hormonal cause, a contributing factor to androgenic alopecia is that hair follicles do not have enough supporting stem cells and fibroblasts, which are essential for anchoring the hair in place. When this reaches a critical mass, there is not enough scaffolding to support the follicle, and the hair will fall out. PRP supports this, but more effective treatment is to inject the scalp with a mega-dose of viable fibroblasts and stem cells using stem cell extract. This patient is in his early 50s. Over the last 10 years, he has experienced increasing thinning of his hair. The patient did not want a hair transplant but was concerned that in the next two years, he would have to shave his head. However, a single treatment, where we took some 2mm biopsies and used a microlyser to separate the graft into a viable colony of fibroblasts, created the result you see below.
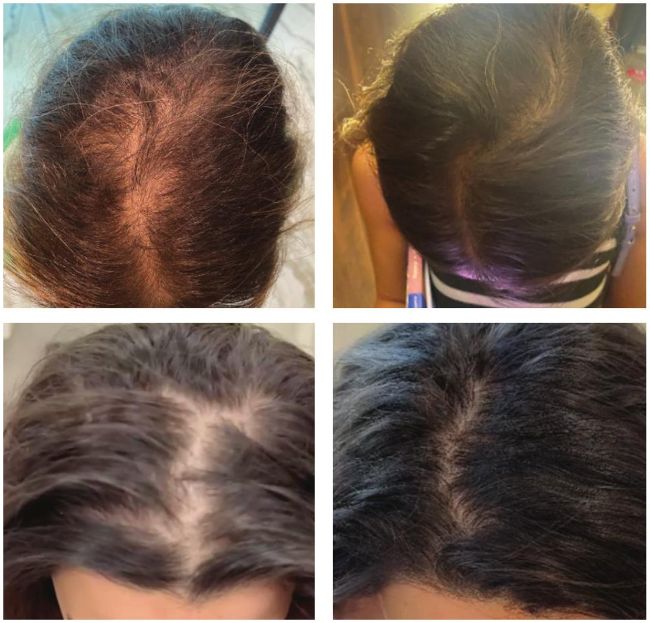
Case study three (before and after) The patient is in her early 30s; she has been suffering from a general thinning of her scalp for a few years and has not sought treatment. We decided to work on a combined plan of exosome-rich plasma and stem cells. We used the T-lab system available in the UK from Hawksley. The results are excellent.
REFERENCES
1. Y. Fan et al.Clinical uses of platelet-rich fibrin in oral and maxillofacial surgery, Dent. Clin. North Am.(2020)
2. Thomas SG. The structure of resting and activated platelets. Platelets, 2019: p. 47–77
3. Chen Y., Shao J.Z., Xiang L.X., Dong X.J., Zhang G.R. Mesenchymal stem cells:Apromising candidate in regenerative medicine. Int. J. Biochem. Cell Biol. 2008;40:815–820
4. Dashore, Shuken; Chouhan, Kavish1; Nanda, Soni2; Sharma, Aseem3. Preparation of Platelet-Rich Plasma: National IADVL PRP Taskforce Recommendations. Indian Dermatology Online Journal 12(Suppl 1):p S12-S23, November 2021
5. Maharani, E. A., &Astuti, D. (2022). Comparison of Single Centrifugation, Double Centrifugation and Turn down-Turn up Techniques for Platelet-Rich Plasma Quality. Althea Medical Journal, 9(3), 180-184.
6. Fujioka-Kobayashi M, Miron RJ, Hernandez M, Kandalam U, Zhang Y, ChoukrounJ (2017) Optimized platelet-rich fibrin with the low-speed concept: growth factor release, biocompatibility, and cellular response.J Periodontol 88(1):112–12
7. Miron RJ, Fujioka-Kobayashi M, Hernandez M, Kandalam U, Zhang Y, Ghanaati S, ChoukrounJ (2017) Injectable platelet rich fibrin (i-PRF): opportunities in regenerative dentistry? Clin Oral Invest 21(8):2619–2627
8. Ehrenfest DM, Rasmusson L, AlbrektssonT (2009) Classification of platelet concentrates: from pure platelet-rich plasma (P-PRP) to leucocyte-and platelet-rich fibrin (L-PRF). Trends Biotechnol 27(3):158–16
9. Miron RJ, Chai J, Zhang P, Li Y, Wang Y, Mourão CF, Sculean A, Fujioka Kobayashi M, Zhang Y (2020)Anovel method for harvesting concentrated platelet-rich fibrin (C-PRF) with a 10-fold increase in platelet and leukocyte yields. Clin Oral Invest 24(8):2819–2828
10. Kobayashi M, Kawase T, Horimizu M, Okuda K, Wolff LF, Yoshie H (2012)Aproposed protocol for the standardized preparation of PRF membranes for clinical use. Biologicals 40(5):323–329
11. Diab, N.A.F., Ibrahim, As.M. &Abdallah, A.M. Fluid Platelet-Rich Fibrin (PRF) Versus Platelet-Rich Plasma (PRP) in the Treatment of Atrophic Acne Scars:AComparative Study. Arch Dermatol Res 315, 1249–1255 (2023)
12. Czop J, Jałowska M. Stem cells in plastic surgery and aesthetic medicine. Advances in Dermatology and Allergology/Postępy Dermatologii iAlergologii. 2023;40(4):504-50
13. White C, Brahs A, Dorton D, Witfill K. Platelet-rich plasma:AComprehensive Review of Emerging Applications in Medical and Aesthetic Dermatology.JClin Aesthet Dermatol. 2021 Nov;14(11):44-57
14. Yıldız, Isa; Görgü, Metin1; Karanfil, Ertuğrul1; Yoldas, Hamit. The Effect of Needle Diameter on Platelet Concentrations in Platelet-rich Plasma Injections. Turkish Journal of Plastic Surgery 33(1):p 17-23, Jan–Mar 2025
15. Arendt-Nielsen, L., Egekvist, H., &Bjerring, P. (2006). Pain following controlled cutaneous insertion of needles with different diameters. Somatosensory &Motor Research, 23(1–2), 37–43
16. Gordon H. Sasaki, Micro-Needling Depth Penetration, Presence of Pigment Particles, and Fluorescein-Stained Platelets: Clinical Usage for Aesthetic Concerns, Aesthetic Surgery Journal, Volume 37, Issue 1, 1January 2017, Pages 71–8
17. Metin Görgü, Ali Gökkaya, Ertuğrul Karanfil, What Is the Adequate PRP Dose for an Effective Treatment? An In Vitro Experimental Study on the Skin, Aesthetic Surgery Journal, Volume 41, Issue 7, July 2021