CLINICAL
Treating acne scarring and pigmentation
Kate Monteith Ross looks at the efficacy of plasma and exosome treatment
This case study explores the synergistic effects of nitrogen plasma and exosome therapy in the treatment of active acne and post-acne scarring. Plasma effectively targets active acne by reducing inflammation and bacterial presence while simultaneously resurfacing the skin to address textural irregularities and scarring. The addition of exosome therapy plays a crucial role in accelerating healing, regulating melanin production, and reducing the risk of post-inflammatory hyperpigmentation.
Results from the case study demonstrated a significant reduction in both live acne and residual scarring, with visible improvements in skin texture, elasticity, and overall quality. The patient exhibited reduced fibrosis, enhanced collagen remodelling, and a more even complexion, with skin tightening effects contributing to a rejuvenated appearance. This combined approach offers a highly effective solution for acne sufferers, improving both immediate and long-term skin health while minimising complications associated with conventional treatments.
INTRODUCTION
Acne scarring is a common and distressing consequence of moderate to severe acne, particularly in cases involving nodules, cysts, papules, and pustules. These inflammatory lesions trigger an immune response, leading to prolonged inflammation that disrupts the normal architecture of the epidermis and dermis. This disruption results in the degradation of key structural components, including collagen, elastin, and the extracellular matrix (ECM), which are essential for maintaining skin integrity and elasticity.1
The wound healing process in acne-affected skin is often dysregulated.2 Fibroblasts, responsible for collagen production, may generate excessive or insufficient Type I and III collagen, leading to abnormal scar morphology.3 Additionally, heightened matrix metalloproteinase (MMP) activity exacerbates the breakdown of ECM proteins, further impairing wound healing and contributing to atrophic scarring. The loss of collagen manifests as various types of acne scars, including ice-pick, boxcar, and rolling scars, which result in permanent textural irregularities.4
Post-inflammatory hyperpigmentation (PIH) is another significant concern, particularly in darker skin tones, occurring due to the stimulation of melanocytes by inflammatory cytokines and UV exposure.5 This leads to persistent discolouration that can be difficult to treat. Furthermore, angiogenesis and abnormal capillary dilation contribute to residual post-acne erythema and redness, prolonging the visible effects of acne even after active lesions have resolved.6
Understanding these pathological mechanisms underscores the need for advanced therapeutic strategies that not only address active acne but also mitigate long-term scarring, pigmentation issues, and vascular changes to restore skin quality and function effectively.
Additionally, acne scarring is among the indications approved by the US Food and Drug Administration (FDA) for treatment, signifying its recognition as a clinically validated condition for medical intervention.
METHODS
The case study focuses on a single male patient who had suffered from live acne, scarring and pigmentation. The patient in the past had treatments with topicals and multiple CO2 laser treatments, which resulted in minimal improvement, persistent fibrosis, scarring, uneven skin tone, and post-treatment pigmentation. The patient underwent a series of three treatments using Neogen Nitrogen Plasma at an energy level of 1.8 joules.
Each session involved the application of two full passes across the entire facial area. Patients were treated with a vertical and horizontal two-step pass to ensure the energy was passed uniformly in the areas of treatment.7 Immediately post-treatment, a topical application of exosome-based therapy was administered to enhance skin recovery and regulate melanin production. The patient was also provided with additional exosomes for topical application the following day to further support the healing process.
The rationale for applying Dermafocus Purasomes immediately post-treatment was based on the principle of transdermal absorption, a process referred to as plasmaporation. This phenomenon occurs when nitrogen plasma temporarily increases skin permeability, allowing for enhanced absorption of topical agents. The application of exosomes directly after treatment takes advantage of this increased permeability, optimising their penetration into the deeper layers of the skin, where they can exert their regenerative effects; this mechanism is supported by evidence from a study published in the European Journal of Medical Research (2024), which explored the impact of cold atmospheric plasma on skin permeability and transdermal drug absorption. The study demonstrated that plasma treatment significantly enhances the skin’s ability to absorb topical substances, reinforcing the efficacy of post-treatment exosome application.8
Pigmentation disorders, such as melasma and post-inflammatory hyperpigmentation, present significant therapeutic challenges due to their chronic nature and tendency for recurrence. Recent advancements in regenerative medicine have highlighted the potential of exosomes, nanosized vesicles secreted by cells, as a novel treatment modality for pigmentation disorders. Exosomes are rich in bioactive molecules, including growth factors which can modulate melanogenesis by regulating melanin synthesis pathways, reducing inflammation, and promoting skin regeneration.9
Treatments were performed at three-week intervals, allowing sufficient time for skin regeneration between sessions. The final clinical assessment and photographic documentation were conducted 50 days after the last treatment to evaluate improvements in scarring, fibrosis, pigmentation, and overall skin quality.
RESULTS
The treatment demonstrated a 39% improvement in surface pigmentation, 14% improvement in sensitivity, 29% reduced pore size, and a 41% reduction in acne and inflammation over the three treatments as quantified by the 3D Visage Skin Analysis System, indicating a significant reduction in post-inflammatory hyperpigmentation and overall improvement in skin health and tonality.
Additionally, a visible lift and tightening effect were observed, particularly around the jawline and neck suggesting enhanced skin firmness and collagen remodelling.
Post-treatment assessment revealed complete resolution of active acne lesions, with no recurrence observed throughout the follow-up period. Fibrosis was visibly improved, contributing to a smoother skin texture with reduced pore size. The overall skin quality appeared more refined, with increased suppleness and uniformity.
The patient reported a shortened recovery period of only three to four days, despite receiving treatment at 1.8 joules, a setting typically associated with a more extended downtime. This expedited healing process suggests the efficacy of exosomes in accelerating post-procedural recovery, minimising inflammation and enhancing skin regeneration.
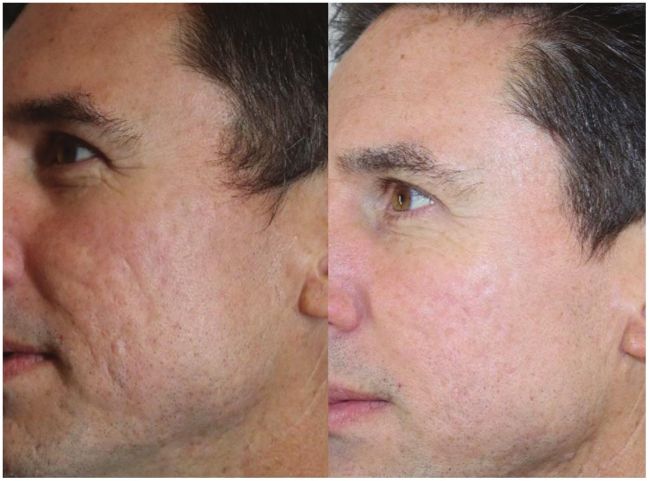
Before and after
CONCLUSION
This case study highlights the efficacy of nitrogen plasma combined with exosomes in treating acne scars, fibrosis, and post-inflammatory pigmentation while also improving overall skin quality. The treatment demonstrated a promising reduction in surface pigmentation, visible skin tightening, improved texture, and reduced fibrosis. The absence of active acne post-treatment further supports the regenerative and antimicrobial benefits of this approach.
Additionally, the shortened downtime of three to four days, despite the use of a high-energy setting (1.8 joules), suggests that exosomes played a key role in accelerating the healing process by leveraging enhanced transdermal absorption via plasmaporation. This finding underscores the potential of combining exosome therapy with nitrogen plasma to optimise skin recovery and minimise post-treatment hyperpigmentation.
Overall, this study demonstrates that nitrogen plasma with exosomes is a highly effective and well-tolerated treatment for acne scarring and skin rejuvenation, offering both functional and aesthetic benefits. Future research with larger patient cohorts is recommended to further validate these findings and establish standardised treatment protocols.
KATE MONTEITH ROSS
Kate Monteith Ross is the founder, clinical director and lead aesthetic nurse of The Clinic by La Ross. She is a member of the British Association of Medical Aesthetic Nurses and the Royal College of Nurses, as well as registered with the Aesthetic Complication Experts and CMAC, as she is passionate about patient safety and building her complications knowledge. Monteith Ross is also the director of Urban Aesthetics Academy UK and is a regional associate trainer for Teoxane, faculty for Dermafocus with a keen interest in combination treatments and full face harmonisation. She is also a KOL for Dermalux, an ambassador for Neogen Plasma and one of the co-founders and directors of The Nurses Network.
REFERENCES
1. Kang S, Cho S, Chung H, Hammerberg C, Fisher GJ, Voorhees JJ. Inflammation and extracellular matrix degradation mediated by activated transcription factors nuclear factor-kappaB and activator protein-1in inflammatory acne lesions in vivo. AmJPathol. 2005 Jun;166(6):1691-9. doi: 10.1016/s0002-9440(10)62479-0. PMID: 15920154; PMCID: PMC1602424.
2. Xu W, Sinaki DG, Tang Y, Chen Y, Zhang Y, Zhang Z. Acne-induced pathological scars: pathophysiology and current treatments. Burns Trauma. 2024 Apr 5;12:tkad060. doi: 10.1093/burnst/tkad060. PMID: 38585341; PMCID: PMC10998535.
3. Kim HY, Im HY, Chang HK, Jeong HD, Park JH, Kim HI,Yi HS, Kim YS. Correlation between Collagen Type I/III Ratio and Scar Formation in Patients Undergoing Immediate Reconstruction with the Round Block Technique after Breast-Conserving Surgery. Biomedicines. 2023 Apr 4;11(4):1089. doi: 10.3390/biomedicines11041089. PMID: 37189707; PMCID: PMC10135880.
4. Cabral-Pacheco GA, Garza-Veloz I, Castruita-De la Rosa C, Ramirez-Acuña JM, PerezRomero BA, Guerrero-Rodriguez JF, Martinez-Avila N, Martinez-Fierro ML. The Roles of Matrix Metalloproteinases and Their Inhibitors in Human Diseases. IntJMol Sci. 2020 Dec 20;21(24):9739. doi: 10.3390/ijms21249739. PMID: 33419373; PMCID: PMC7767220.
5. Lawrence E, Syed HA, Al Aboud KM. Postinflammatory Hyperpigmentation. [Updated 2024 Nov 25]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan-.Available from: https://www.ncbi.nlm.nih.gov/books/NBK559150/
6. Yang Y, Wu X, Liu W. Scar Symptom: Erythema and Thickness. 2020 Dec 8. In:Téot L, Mustoe TA, Middelkoop E, et al., editors. Textbook on Scar Management: State of the Art Management and Emerging Technologies [Internet]. Cham (CH): Springer; 2020. Chapter 11. Available from: https://www.ncbi.nlm.nih.gov/books/NBK586055/
7. Professor Syed Haq, Energy Work (UK: Aesthetic Medicine, 2018)
8. European Journal of Medical Research, 29(1). Available at: https://eurjmedres.biomedcentral.com/articles/10.1186/s40001-024-02088-9).
9. (Lo Cicero, A., Delevoye, C., Gilles-Marsens, F., Loew, D., Dingli, F., Guéré, C., André, N., Vié, K., Van Niel, G. and Raposo, G., 2015. Exosomes released by keratinocytes modulate melanocyte pigmentation. *Nature Communications*, 6, p.7506. DOI: 10.1038/ncomms8506.)