INFRAORBITAL MARKING
Making a MARK
Dr Uche Aniagwu on advanced marking of the infraorbital region when using HA fillers
DR UCHE ANIAGWU
DrUcheAniagwu MBBS, MSc, BSc is aUniversity ofOxford graduate, and aesthetics doctorfocused on the infraorbitalregion. In addition to being an author, DrUche is an internationalspeakerand trainer, with hisTearTroughAcademy being world-renowned. He is also the founderofClinic Mate, a series ofproducts designed to promote more consistent and safe planning practices in injecting. You can follow him on Instagram: @clinicmate and @drucheuk.
L ike most cosmetic injections, the infraorbital region tends to follow the standard steps that lead to consistently good and safe outcomes: Assessment, Planning and Execution (APE). Yet, we’ve seen a lean toward emphasising only the Execution phase. The uncanny thing about these phases of treatment is that a suboptimal outcome in one phase leads to greater demand in the following phase, and often that demand is unmet, leading to suboptimal injecting outcomes.
The APE system may carry its greatest significance in the infraorbital region, which is notoriously difficult to treat and presents fine margins in which to execute. For the purpose of this article, we will be focusing on the “Planning” phase to demonstrate exactly how the marking up of the infraorbital region can be the difference between consistently non-complicated outcomes, or consistently poor outcomes.
As aforementioned, the planning phase may have the most value in the tear trough region, where the margins for error are so small. But what exactly does planning in this area look like? Granted, the correct answer to that question really depends on who is discussing or teaching, as an injector’s planning approach in the tear trough is directly correlated to their injection technique.
For the sake of this article, I will be providing the structure for infraorbital injection planning as per my injecting technique. I have used this technique on more than 500 patients and have taught it to over 200 injectors/surgeons worldwide, with its foundation being the DUTTA classification.
The first thing I advise injectors to consider when they are marking up the infraorbital region as part of their planning phase is to consider their objectives as twofold. Objective number one is to ensure a safe approach when injecting the region. While complications are statistically unavoidable, a thorough understanding and mapping of key anatomy can help to massively reduce the risk of serious medical complications. The second objective is to provide a reliable and desirable cosmetic outcome for the infraorbital region. This, once again, requires a good understanding of the local anatomy, but also calls upon the injector to have an understanding of their product of choice and how it interacts with the facial region.
I encourage anybody reading this to fortify their anatomical knowledge of the region in order to truly appreciate the contents of this article; some may find it useful to return to the article following some further reading. With that being said, we will split the marking of the face into ‘safety’ or ‘cosmetic’.
My final word, before we go into the planning nuts and bolts, is to consider the tools at your disposal. Where possible, I encourage practitioners to make use of ultrasound devices to guide their injections, but more importantly, I encourage injectors to have reliable marking tools that do not encourage one to take short-cuts. The reality is that not everyone reading this article will have access to an ultrasound device or have the skill to utilise it, but every practitioner can rely on anatomical knowledge and good marking up of the face – that’s base one.
SAFETY
Firstly, let’s discuss the one time I don’t advise marking up the patient. It is not advisable to progress a cannula or needle superiorly beyond the orbital rim when injecting the tear trough with hyaluronic acid (HA) filler. Therefore I suggest practitioners do NOT draw the inferior border of the orbital rim. Instead, palpate for it when injecting. Marking the skin in this instance can be misleading as to the position of the inferior orbital rim, and the structure is robust enough that palpating it and using one’s finger as a barrier is adequate.
Mid-Pupillary Line (MPL)
The MPL is an important safety marker for us injectors when treating the infraorbital region. Accounting for anatomical variation, the Infraorbital Artery lies in the medial limbus line and poses the greatest threat of vascular complications when augmenting the medial cheek with boluses on the periosteum. I encourage injectors not to inject medial to the MPL when administering a medial cheek, periosteal bolus. There are rare circumstances when this guidance may be compromised, but introducing those concepts here may serve to increase appetite for risk – in short, no periosteal injections medial to the MPL.
Lid Cheek Junction (LCJ)
The LCJ is the surface anatomy representation of the orbitomalar ligament and signifies the transition from “eye zone” to “cheek zone”. The advanced injector uses this border as the superior ceiling of where any high G prime products will be placed. Lymphatic drainage above the LCJ (malar septum) is poor, and the septum here is relatively impermeable. As such, a high G-prime filler in the eye zone will massively predispose the patient to develop postinjection persistent infraorbital oedema. This is a real challenge to manage, so remember to keep your high G-prime products beneath the LCJ.
Malar Mounds (MM)
Malar mounds are swelling, often visible in the lateral part of the infraorbital region. They, technically, sit in the cheek zone and correspond to the pre-zygomatic space. Unfortunately, for many patients, this area can bulge secondary to poor lymphatic clearance or fat hypertrophy. The region is prone to further swelling, with many cases not resolving. As part of planning, injectors are encouraged to mark out any visible malar swelling on the patient. It is normal for malar mounds to not be obvious in certain lights and so I suggest assessing this region from different vantage points around a fixed patient. Inadvertent HA in this region, bruising, and general trauma in the MM can lead to long-lasting oedema. The key is to avoid any malar oedema or malar mounds when planning your injection path, including your entry point. By clearly demarcating this deformity, practitioners can reduce their post-treatment complication rate.
Deep Medial Cheek Fat (DMCF)
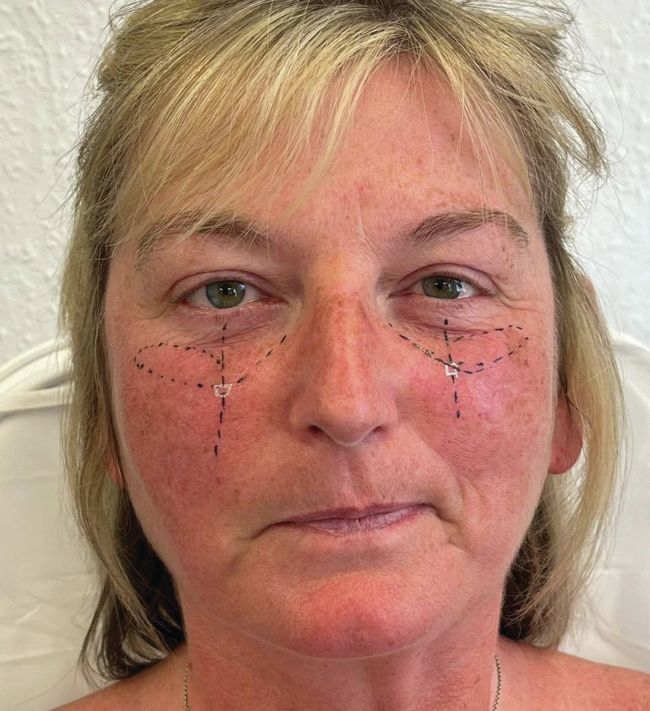
It is commonly documented that managing the cheeks is typically the first step in managing the tear trough. This is a vague simplification of a treatment approach that requires injectors to know how augmenting different compartments of the cheek impact the appearance of a tear trough deformity. There is a multitude of approaches, but, in my experience, the most important cheek point is in the medial cheek, and this is often true of all vectors. Again, if you find that some of this terminology is foreign to you, it may be pertinent to familiarise yourself with the anatomy and assessment of the infraorbital region and then revisit this article. So why is planning /marking of the patient important in this context? Well, we are not just augmenting any part of the cheek. In fact, injectors should look to support the DMCF right below the transition from eye zone (suborbicularis oculi fat – SOOF) to cheek zone (DMCF). Injecting in this region provides maximal anterior projection and support for the often descending orbitomalar ligament. This injection point is a consistent game changer and simply requires that the ‘safety’ markings have been adequately drawn. Ensuring it’s tight to the LCJ, while not crossing into the eye zone gives the optimal result. The advanced injector will map out an injection path which accounts for upward needle angulation beneath the skin.
Tear Trough Groove (TTG)
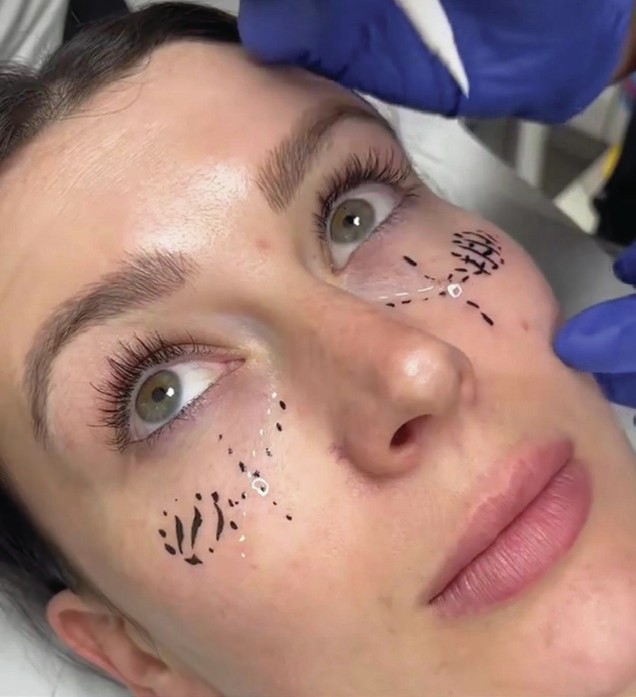
Mapping the TTG injection path requires focus and precision, as only millimetres separate a good result from a potentially troublesome one. When planning the injection path for this area, the markings must serve only as a guide. I encourage injectors to check and re-check their cannula position when in the TTG. However, spending the time mapping out an accurate injection path here will aid in your entry point decision-making. The shortest distance between two points is a straight line, and that is just as true when injecting the TTG. An entry point that allows for easy and direct injecting across the length of the TTG will result in the fewest errors. A tip I give to my students is to have the patient look upwards as you mark out the TTG; this will often exaggerate the groove and make planning the injection path simpler. By focusing more on my planning and approach to the TTG, I was able to see my average use of 0.4ml of HA filler per eye reduce to 0.25ml of HA filler per eye. This led to a reduction in complications without a reduction in patient satisfaction. It is worth remembering that the region is very small and that it is tethered by a ligament, so injecting into this area should be conservative and only acts as a camouflage, not an untethering of the tear trough ligament.
CONCLUSION
Developing a thorough routine for planning infraorbital injectables will bring greater consistency to an area of the face that is notoriously unpredictable. Importantly, our balance between confidence and anxiety as practitioners is extremely important to our wellbeing and, consequently, performance. Consistent planning habits serve to give more confidence while lowering anxiety. Furthermore, injectors should ensure they have the correct tools to complement their system, as this leads to a compound effect, yielding long-term injectable success in the tear trough.