When the unthinkable happens
Dr Anna Hemming recounts how she handled a particularly challenging complication
At 1.42pm one Thursday lunchtime, the notification of A an email innocently arrived on my screen. As I was between patients I saw the first few words: “I didn’t want to bother you, but I thought I would check, is this normal? I have been applying a cold compress and taking ibuprofen, but wanted to check if there is anything else I can do.”
Normally, I would leave my experienced team to deal with all patient emails, however this was a patient I had treated with dermal filler the previous day and, knowing the patient, something within the email didn’t seem right. Moments later, I was on the phone to her, asking if she was in pain (no), whether there was any blanching (yes) and various other questions. A photo immediately arrived of the kind we have all seen at complications training. This was not normal, and we needed to bring her in. Being 90 minutes away from the clinic, she arrived as soon as she possibly could.
In the meantime, clinic ran as normal, patients were seen, and, in the back of my mind, my complications file was being pulled out and the algorithm for vascular occlusion (VO) run through. By the time the patient arrived in clinic, I had reviewed her notes (after images were totally normal, no mottling and no altered capillary refill time (CRT), reviewed the ACE guidelines for VO and had all the emergency drugs at hand, just in case.
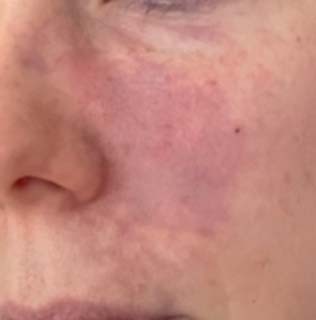
Image 1 was the image sent to clinic, clearly showing mottling (livedo reticularis). The arteriole flow to the skin has been affected, blocking perfusion to the capillary bed, causing the tissue to blanch and display pallor and then mottle. With skin hypoxia visible and some greying to the skin too indicating tissue infarction, it was paramount that the patient came to clinic as soon as possible
My patient is a 42-year-old with asymmetry. I had treated her 12 months previously with dermal filler with great success. Her 12-month review had recently passed and there was distinct volume loss to the temple, medial and lateral suborbicularis oculi fat (SOOF), as well as the tear trough. Her left side was always more depleted than the right and we had a plan to stabilise the deep fat pads, bringing deep alignment and then review, to address the tear trough depressions.
At the review, the tear trough filler was used to lift the under eye, especially on the left. The immediate results were lovely, there was no pain or unusual after-effects, until seven hours after the filler, when the patient noticed some numbness (she thought initially it was the local anaesthetic from the treatment). In the evening, the area was slightly pinker, but it wasn’t until the next day and 24 hours after treatment that she emailed, as the area was still a bit pink.
HOW TO ASSESS POTENTIAL VO
Patients are often in pain, have reduced CRT in the area and surrounding skin, and display pallor initially and then mottling.
Immediate action is required if there is any suspicion of VO or spasm of the nerves causing hypoxia to the skin. Rapid action is necessary to reverse the hypoxia before necrosis establishes, leading to tissue breakdown and wounds.
In this patient, the pallor stage was not visible in clinic, presentation occurred at 24 hours in the livedo reticularis phase.
Phases of a VO
1. Pallor – Occurs with immediate blockage of an arteriole as the blood flow is interrupted and blocks tissue perfusion. Lasts seconds – or persists longer.
2. Livedo reticularis – A mottled pattern appears on the skin from the build-up of deoxygenated blood from the venous network. Can occur rapidly, lasting 24-36 hours.
3. Pustules – Typically at 72 hours due to the reduction in pH and sweat, along with metabolic changes due to hypoxia allowing staph. aureus bacterial over production.
4. Coagulation – Indicating necrotic change and can occur before pustule formation. Caused by worsening hypoxia, skin darkens as cell lysis occurs and there is leaking of blood into the tissues. Skin tissue remains firm due to the coagulative necrotic process.
5. Tissue destruction – Skin breaks down due to a build-up of denatured structural proteins (collagen, fibrin, elastin) neutrophils, bacteria, and haemoglobin. Devitalised tissue is initially moist creamy/yellow or green (slough) and then becomes black (dark) and dry. This occurs days after the occlusion.
HOW TO TREAT A VO?
• Stop treatment (if they are with you) and inform them about what is happening
• Check and video CRT on both affected and unaffected skin for comparison
• If CRT is delayed, it indicates vascular compromise
• Massage the area firmly, applying heat to encourage vasodilation
• Assess
• Get help
• Hyaluronidase (do not skin test, ensure anaphylaxis medications are at hand just in case)
• Disinfect the skin
• Reconstitute 1500 hyaluronidase in 1ml NaCl 0.9% or 1-2% lidocaine
• Infiltrate 1500IU by needle or cannula over the course of the affected artery and wider area of ischemia. More than one vial may be needed
• Apply heat and massage area vigorously (helps mechanical breakdown of HA)
• Assess CRT and if >3 seconds repeat hyaluronidase hourly
• Review patient daily
• Clinical resolution may be required over the following days to avoid deterioration
• Make detailed notes and take images and videos
• Advise insurers so they are aware of the situation.
Medications that may help Aspirin or Clopidogrel 300mg stat and 75mg per day.
The following may also help reverse compromise:
• Nitroglycerin paste
• Hyperbaric oxygen
• Steroids only if clinical indication
• Wound management
• Antivirals if tissue has started to break down
• Antibiotics.
PROGRESS OF THIS PATIENT’S VASCULAR EVENT
On arrival in clinic the day after dermal filler treatment, we talked through the situation openly. She was not in pain; her CRT was sluggish in the area treated and the surrounding vascular pathway. Livedo reticularis was present with non-blanching erythema and even greying of the tissue in the distal vascular pathway.
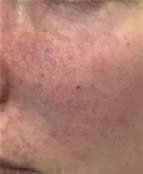
Image 2 In clinic presentation 24 hours after dermal filler treatment It was clear a vascular event had happened, although delayed and without the typical pain experienced.
My gut feeling was the vessel had experienced a spasm, affecting the distal branches delivering oxyhaemoglobin to the skin.
With open discussion we planned her treatment. Immediate aspirin, hyaluronidase and antibiotics were started due to the delayed presentation, to try to decrease pustule formation and necrosis.
Day two
As I was attending a conference 10 minutes away from her the following day, we planned to review at the conference, where I arranged a private room and place where we could treat her again. 1500IU of hyaluronidase was administered, exosomes were started topically and after consulting with colleagues a short course of prednisolone commenced.
Day three
We arranged hyperbaric chamber sessions starting the following day along with review and a further 1500IU as the area was still firm. Tiny white pustules started to appear in the apical triangle to the side of the nose. The erythema was shrinking and the numbness was improving.
Day four
The area was injected one last time with 1500IU hyaluronidase and a further hyperbaric chamber session attended. Bruising from hyaluronidase flooding can be seen in the filler treatment area.
Day five
A small area in the apical triangle has potential for necrotic breakdown.
Day seven
The patient has a further hyperbaric chamber session. The bruising, inflammation and vascular compromise settled and the apical triangle crusting was mildly better.
Day 10 - Further hyperbaric chamber session
Day 12
Day 16
Day 45
Day 12, 16 and 45 saw huge improvements in the look and feel of skin, with reduced numbness. The patient was left with a small amount of erythema. The apical triangle remained intact and didn’t breakdown.
IN TOTAL
• 9 appointments
• 4 x 1500 IU hyaluronidase
• Aspirin 300mg stat, 75mg OD
• Flucloxacillin 500mg QDS 7/7
• Prednisolone 40mg OD 5D
• 5 hyperbaric chamber sessions
We have our next review planned and aim to help resolve the erythema in completion with laser genesis or excel V+ treatment.
The patient is hugely relieved that we were able to get on top of the vascular event as soon as we were aware of it. She is happy with our treatment.
DR ANNA HEMMING
Dr Anna Hemming is a fully qualified general practitioner and medical skin doctor with over 22 years of experience. She owns Thames Skin Clinic in Twickenham, which she founded in 2019. Dr Hemming has a background in anaesthetics and emergency medicine, serving with the Royal Army Medical Corps as a captain and spending seven years as a general practitioner at Buckingham Palace.