PLATELET-RICH FIBRIN
New blood
PRF offers skin–rejuvenation results far beyond that of PRP, says Dr Beena Harkison
DR BEENA HARKISON
Dr Beena Harkison graduated in Dentistry from the University of Witwatersrand in South Africa. She also has a Master’s degree in Implantology (MSc Implantology) and was a Research Fellowship Student at the South African Medical Research Council. In 2011, she achieved an MBA from Imperial College, London and graduated with Merit. Dr Harkison has also undertaken extensive training in the field of facial aesthetics using patients’ own blood constituents and growth factors under the tutelage of Dr Cleopatra Nacopoulos. She currently practices at The Courtyard Clinic in Chertsey, Surrey. Follow her on Instagram: @beenaharkison
Platelet concentrates, specifically platelet-rich plasma (PRP), have been widely used in surgical procedures for joint and wound healing, and more recently, as a topical concentrate in facial aesthetic procedures. Since PRP was made famous by Kim Kardashian more than 10 years ago when she posted a picture of herself undergoing a so-called “vampire facial” on Instagram, the latest generation of platelet concentrate, platelet-rich fibrin (PRF), has emerged in facial aesthetics. There are key differences between PRP and PRF, and I believe that PRF has preceded PRP in terms of its benefits for facial rejuvenation .
PRP VS. PRF
PRP is the first generation of platelet concentrates, while PRF is a second generation developed by Choukroun et al. 1 because of legal restrictions on blood handling. PRP contains additives, typically anticoagulants, but may also contain other unnatural products which might inhibit wound healing, 2 while PRF does not contain any additives or anticoagulants. PRF contains platelets, leukocytes, cytokines and adhesive proteins including fibrinogen, fibronectin, vitronectin and thrombospondin-1. 3
“The presence of white blood cells that secrete a large quantity of growth factors is a key feature of PRF”
The presence of white blood cells that secrete a large quantity of growth factors is a key feature of PRF. The polymerisation of the fibrin produces a three-dimensional crosslinked fibrin matrix which serves as a binding site for both platelets and growth factors. By increasing the local concentration of growth factors at a specific tissue location, PRF promotes tissue regeneration by closely mimicking the wound repair process over a prolonged period of time. The ultimate result is a healing matrix that possesses unique mechanical properties – distinctly different from PRP.
If we look at growth factor release over time, PRP releases significantly higher levels of growth factors at earlier time points, while PRF displays continual and steady release over a 10-day period. 4
PRP doesn’t have standardised protocols for centrifugation, unlike PRF which uses a low speed centrifugation concept (LSCC), which, in turn, increases the concentration of platelets and leukocytes, and therefore the release of the many growth factors required for wound healing. In addition, Miron et al (2017) showed that PRF demonstrated the ability to release higher concentrations of various growth factors and induced superior fibroblast migration and expression of PDGF, TGF-ß, and collagen-1 when compared to PRP. 5
It is for these reasons that PRF now supersedes PRP as an autologous platelet concentrate, not only for maxillo-facial and dental applications, but also for facial aesthetics and hair rejuvenation.
PREPPING FOR TREATMENT
Like with all treatments, PRF procedures start with a consultation. PRF is indicated for:
• Natural collagen induction
• Skin tightening and firmness
• Improvement of fine lines and wrinkles
• Treatment of acne scars
• Improvement in skin tone and texture
• Minimising open or enlarged pores
• Improvement in skin pigmentation
• Outside of the facial aesthetics zone, PRF can also be used to treat stretch marks and hair loss or alopecia.
An important part of the consultation aside from the presenting complaint is obtaining an understanding of a patient’s lifestyle and dietary habits. Because PRF is a blood-derived product, the quality and quantity of plasma – and therefore the treatment outcome – will depend on the patient’s lifestyle. In patients that smoke or drink a lot of alcohol, the improvements are often not as great as in individuals that do not smoke, limit alcohol intake, drink plenty of water, eat fruits and vegetables and do regular exercise. In other words, PRF is ideally suited for those people with a healthier lifestyle, not only for obtaining improved treatment outcomes of their presenting complaint, but also for maintaining that result for a longer period of time.
As I say to all my patients, “Rubbish in, rubbish out!” If a patient is not able to adjust their lifestyle or if they are expecting instantaneous results, then PRF treatment is not the right treatment for them. Generally, a patient would start to see some results after the second or third session, so it’s important to set expectations that instantaneous results are unlikely, even though they may see some improvements after the first session. It’s also for that reason that I would recommend four sessions to all patients, with each session spaced four-to-six weeks apart. Thereafter, depending on their lifestyle habits, they would then fall into a maintenance schedule which varies between four to six months for top-up sessions. If the patient wishes to proceed with the treatment, then they are booked in for the first session. Consent forms will be emailed to them to read beforehand at home.
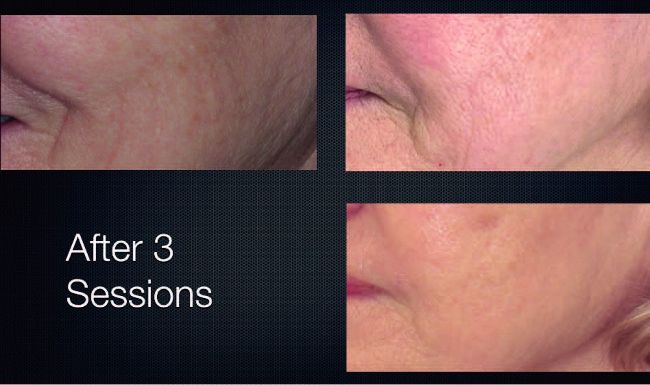
Images courtesy of Dr Beena Harkison
The patient is instructed to stop using any creams with salicylic acid, Vitamin C or retinoids five days prior to the first PRF appointment. The patient is also instructed to take 1g paracetamol and to apply a topical anaesthetic cream onto their face and neck an hour before the appointment time. Patients are also encouraged to drink plenty of water prior to the appointment to allow the veins to become distended, allowing for easier blood collection.
BEST PRACTICE PROTOCOL
The steps taken at the treatment appointment are as follows:
1. Check that the consent is signed, and the patient has applied the topical anaesthetic.
2. Take photographs – this is important as the patient often forgets their starting point and referring back to these photos is a good way to remind them of the improvements over time. The minimum range of photos are frontal, left and right profile, and left and right 45-degree angled. Any particular areas of concern highlighted by the patient can also be taken at a higher resolution.
3. Blood collection – generally four-to-six 9ml tubes are sufficient for the face and neck region. The blood is centrifuged with a Choukroun PRF Duo Quattro System machine at 700rpm for five minutes, as per Choukroun and Ghanaati PRF protocols. 7
4. While the blood is being centrifuged, the skin on face and neck is cleansed and disinfected. I recommend all patients attend the clinic without make-up. As PRF contains no anticoagulants, it’s important to be prepared for the next step to avoid coagulation of the PRF concentrate.
5. As soon the blood has been separated in the centrifuge, the plasma is drawn up and liberally applied onto the skin. The plasma is allowed to penetrate the skin through microneedles. Microneedling with a Dermapen 4 device over the PRF-rich plasma stimulates the production of new collagen and elastin, hence it is indicated for a number of different conditions, as listed above. By adjusting the needle depth, microneedling can also treat hyperpigmentation or even stretch marks.
As the microneedling pen tips are extremely small, penetration around the eyes is also possible, which offers advantages over other treatments as the area around the eyes tend to bruise and bleed easily. Microneedling also has the advantage of a deeper, more even or uniform penetration of the PRF concentrate through the microchannels created by microneedling, when compared to multiple intradermal or microinjections. 7
6. Each area of the face or neck needle depth is documented on a face mapping chart, which can either be replicated at subsequent PRF appointments or adjusted depending on the results seen at the next appointment.
7. Following microneedling with PRF, the patient is positioned for 20 minutes under a LED light (I use the Genosys GENO- LED) to potentiate the effects of PRF with microneedling. Specifically, the red wavelength promotes skin cell regeneration, improved blood circulation, pain relief and activation of active ingredients. The blue wavelength encourages the destruction of acne bacteria, reduction of skin breakouts and inhibition of sebaceous glands. The green wavelength improves hyperpigmentation and sensitivity, and the yellow improves rosacea, erythema and herpes zoster in its early stages. For patients with both skin-regeneration and hyperpigmentation needs, either two 20-minute or two 10-minute sessions can be provided, alternating red and green wavelengths.
8. The patient is instructed to avoid touching their face and neck for the remainder of the day and to only wash their face the next morning, which allows the PRF to work overnight. The usual post-microneedling instructions are also provided in a written form (avoiding alcohol, saunas, swimming pools, direct sunlight, hot showers/ baths, creams with retinoids/vitamin C/salicylic acid can be resumed five days after the appointment).
“Because PRF is a blood– derived product, the quality and quantity of plasma – and therefore the treatment outcome – will depend on the patient’s lifestyle”
9. Subsequent sessions are booked fourto-six weeks apart. Once the fourth session is completed, the patient is advised to attend either three or four times per year for maintenance or top-up sessions.
WHAT’S NEXT?
Imagine being able to predict whether a person will have a good outcome with PRF treatment. I believe this will become established practice in the coming year. If patients are to part with their hard-earned money for any treatment, being able to advise them how successful it’s likely to be is almost expected.
Integrating DNA tests prior to PRF treatment would enable us to indicate if the patient has a genetic predisposition to collagen breakdown or repair, melanin production and thus hyperpigmentation, inflammation and sebum regulation; as well as DNA repair following exposure to UVA/ UVB rays, and so on. If both patient and practitioner had access to this information prior to PRF treatment, they would not only be able to predict how successful the PRF treatment is going to be, but also how many sessions would be required, how often the maintenance sessions would need to be and what topical products and dietary changes are most likely to positively influence the longevity of the PRF treatments.
This vision is actually a reality. I have had DNA analysis on my own skin, and will be introducing this predictive testing to my practice, which I believe will have a significant effect on the successful uptake for PRF - and other treatments.
REFERENCES
1. Budamakuntla L, Loganathan E, Suresh DH, et al. A Randomised, Open-label, Comparative Study of Tranexamic Acid Microinjections and Tranexamic Acid with Microneedling in Patients with Melasma. J Cutan Aesthet Surg. 2013;6(3):139-143. doi:10.4103/0974-2077.118403.
2. Choukroun, J.; Diss, A.; Simonpieri, A.; Girard, M.O.; Schoeffler, C.; Dohan, S.L.; Dohan, A.J.; Mouhyi, J.; Dohan, D.M. Platelet-rich fibrin (PRF): A secondgeneration platelet concentrate. Part IV: Clinical effects on tissue healing. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. Endod. 2006, 101, e56–e60.
3. Choukroun, J.; Diss, A.; Simonpieri, A.; Girard, M.O.; Schoeffler, C.; Dohan, S.L.; Dohan, A.J.; Mouhyi, J.; Dohan, D.M. Platelet-rich fibrin (PRF): A second-generation platelet concentrate. Part V: Histologic evaluations of PRF effects on bone allograft maturation in sinus lift. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. Endod. 2006, 101, 299–303.
4. Ghanaati, S.; Mourão, CF.; Adam, EH.; Sader, R.; Zadeh, HH.; Al-Maawi, S. (2019). The role of centrifugation process in the preparation of therapeutic blood concentrates: Standardization of the protocols to improve reproducibility. 2. 41. 10.4103/GFSC.GFSC_15_19.
5. Grecu AF, Reclaru L, Ardelean LC, Nica O, Ciucă EM, Ciurea ME. Platelet-Rich Fibrin and its Emerging Therapeutic Benefits for Musculoskeletal Injury Treatment. Medicina (Kaunas). 2019 May 15;55(5):141. doi: 10.3390/ medicina55050141. PMID: 31096718; PMCID: PMC6572609.
6. Miron RJ, Fujioka-Kobayashi M, Hernandez M, Kandalam U, Zhang Y, Ghanaati S, Choukroun J. Injectable platelet rich fibrin (i-PRF): opportunities in regenerative dentistry? Clin Oral Investig. 2017 Nov;21(8):2619-2627. doi: 10.1007/ s00784-017-2063-9. Epub 2017 Feb 2. PMID: 28154995).
7. Miron RJ, Chai J, Fujioka-Kobayashi M, Sculean A, Zhang Y. Evaluation of 24 protocols for the production of platelet-rich fibrin. BMC Oral Health. 2020;20(1):310. Published 2020 Nov 7. doi:10.1186/s12903-020-01299-w.