PERIOCULAR COMPLICATIONS
Keep an eye on it
Dr Rachna Murthy and Prof Jonathan Roos of FaceRestoration explain the most common periocular complications and how to avoid them
DR RACHNA MURTHY
Dr Rachna Murthy BSc(Hons) MBBS FRCOphth completed her post-residency fellowship training at Moorfields Eye Hospital, the Craniofacial Unit at Chelsea & Westminster Hospital and the Royal Victorian Eye and Ear Hospital in Melbourne, Australia. She has provided quaternary oculoplastic care for the East of England and sits on the board of Royal Society of Medicine’s Opthalmology section. Follow her on Instagram: @drrachna_murthy
JONATHAN ROOS
Prof Jonathan Roos PhD FRCOphth co-founded FaceRestoration clinic in London with Rachna Murthy. He is a Cambridge, Harvard and Moorfields-trained academic and consultant eye surgeon specialising in periocular cancer, orbital pathology and cosmetic lid surgery. He has published in excess of 50 papers and contributes book chapters on topics including aesthetic management of thyroid eye disease and nasolacrimal duct obstructions. Follow him on Instagram: @drjonathanroos
Eyes are a key feature of facial attractiveness and for communicating expressed emotion. 1 This area is the first to be affected by intrinsic ageing and extrinsic factors such as eye make-up use, sunlight, blue light exposure, pollution and smoking. As a result, it is the area that receives the most attention statistically for enhancement, restoration and rejuvenation, with blepharoplasty coming second only to rhinoplasty for aesthetic surgical procedures; while periocular botulinum toxin treatments are the number one choice for aesthetic non-surgical rejuvenation, followed closely by facial fillers and energy devices. 2
As the demand increases for treatments to this area, the market is quick to respond with various non-surgical modalities to tighten skin, disguise dark circles, and fill so-called tear-trough “deformities”. Even surgical blepharoplasty, which would be the remit of an oculoplastic or specialist facial plastic surgeon, is now offered as part of the repertoire of many generalists and even non-surgeons. It is no wonder then that we are seeing more complications in a largely unregulated market for cosmetic filler, and where a “cookie cutter approach” to periocular surgical restoration is often found.
The periocular area is also the most delicate, with the thinnest skin in the body – less than 1mm in places. 3 The clear window of the eye, the cornea, is the most densely innervated structure in the body, 4 and is 600 times more sensitive than skin,5 while the blood vessels in the eye socket supply the vision. The anatomical complexity of the area is also an important factor.6 There are normal anatomical structures which can change with age, but that can also be damaged inadvertently by the unwary through surgical and non-surgical treatments.
Close attention should be paid to the lacrimal gland which produces tears to protect the ocular surface, the orbital septum, a thin cellophane like fibrous sheet that holds the orbital fat cushioning the eye in its place; and the lateral canthal tendon that supports the outer corner of the eyelid against the orbital bone. These structures are all critically important in the assessment and appropriate choice of treatment to give the optimal outcome and in the prevention of complications for patients. A prolapsed lacrimal gland can be mistaken for orbital fat and cut away, leaving the patient with a chronically uncomfortable dry eye, with resultant risk of corneal ulceration and vision loss.
ENERGY-BASED DEVICES
Non-surgical blepharoplasty using energy devices aimed at avoiding surgical cutting and reducing cost for the patient can be helpful in the patient that wants to avoid surgery and has only mild surplus skin without fat or lacrimal gland prolapse, 7 but a patient’s expectations will not be met if there is anything more than mild dermatochalasis. Plasma fibroblast skin tightening can have significantly more downtime, uncontrollable swelling and only mild to moderate tightening of the skin when compared to a bespoke blepharoplasty, which can address fat pads, lacrimal gland, skin crease position and brow support at the same time. We have found clinically that the resultant inflammation that causes tightening of the skin also causes thickening and rubbery adherence to the layers underneath, making later surgery more difficult.
“It is no wonder that we are seeing more complications in a largely unregulated market for cosmetic filler”
Radiofrequency devices that can improve subcutaneous collagen have gained significant popularity, here thermal energy is directed below the superficial dermis; unlike Plasma, 8 the result is uniform, volumetric, and deep heating. Unlike ablative lasers, which convert light into heat, in monopolar radiofrequency, electric current is converted to heat by tissue resistance.9 There is a risk, however, that previously placed HA filler is broken down. In the periocular area, blepharochalasis and oedema can be worsened initially or unmasked from thermally-induced collagen contraction and a continued progressive inflammatory wound-healing response.
When performing periocular treatments with energy devices and laser, the ocular surface should be protected with topical anaesthesia in the form of eye drops and a protective contact lens or eye shield. Without experience in assessing the eye, appropriate anaesthesia and inadequate ocular protection, there is a risk of corneal injury and damage, and potentially deeper ocular damage. 10 With good technique, however, these adverse events can be avoided.
BOTULINUM TOXIN
Botulinum toxin is a prescription-only drug and is relatively safe – despite being the most popular non-surgical intervention, complications are rare and transient. The most common misconception by patients of periocular toxin is that it can be used to “lift” the brows. As toxin weakens muscles, it is able to weaken the depressor muscles of the eyebrow, allowing unopposed action of the lifting muscle (the frontalis). Thereby, treating the glabellar area and crow’s feet can allow unopposed action of the frontalis and achieve the appearance of lifted brows. Similarly, treatment of the horizontal lines in the forehead weakens the frontalis and can “drop” the eyebrows.11
When a patient has significant dermatochalasis (excess hooded skin), treatment to the forehead lines should be avoided as this will result in ptosis of the eyebrow, worsening the hooding and resulting in an unhappy patient for three months while the toxin effect wears off.
True eyelid ptosis is much rarer and is usually due to too-deep treatment in the lateral glabellar area, too-diluted toxin and migration to the eyelid lifting levator muscle. When patients have underlying oedema in the periocular area, this can be made worse due to weakening of the orbicularis muscle which aids lymphatic drainage.
With correct assessment of the patient’s underlying anatomy and indication, good technique and appropriate dilution of toxin, these complications can be largely avoided. It is important to counsel patients about the pros and cons of the different options and if it is not in the patient’s best interest to have a non-surgical option, a referral for a surgical opinion is advisable.
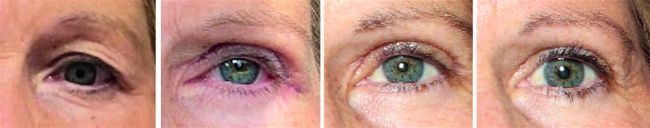
Patient with dermatochalasis and post-filler and toxin complication, managed with surgical blepharoplasty under local anaesthetic. Images courtesy of FaceRestoration.
DERMAL FILLER
The most common complications arise with the use of dermal filler, most of which are self-limiting, such as swelling and bruising, as there is a vast and intricate network of vessels under the skin. Globally, over 8 million filler injections are given every year and over 2.7 million injections were given in the US in 2019 alone. 12 Hyaluronic acid-based fillers are the most popular and this is also the case in our practice, as they have an excellent safety profile and are reversible with hyaluronidase if required. Although the most feared complication among patients and practitioners is vascular occlusion causing vision loss or stroke, this is extremely rare 13,14 – with a relative risk of between 1:100,000 and 1: 1,000,000, there is a greater chance of being struck by lightning.
“If it is not in the patient’s best interest to have a non– surgical option, a referral for a surgical opinion is advisable”
The highest risk areas based on the literature are from filler injections to the nose, forehead and glabellar, where there is direct communication with the retinal arterial circulation, however injections to any part of the face will carry a risk due to multiple communications (anastomoses) between arteries that allow small filler emboli to pass into the eye circulation. Knowledge of the anatomy and good technique in high-risk areas can avoid this complication.
Vision loss is usually immediate and requires early intervention in a specialist eye unit. Treatment of this rare complication is based on consensus and we have previously published guidelines.15,16 Simple measures such as ocular massage, hypercapnoea, reducing the intraocular pressure; and treating the injection site and supratrochlear/supraorbital areas with hyaluronidase can help to dislodge emboli in the retinal circulation.
Hyaluronidase given to the retrobulbar space has been shown to be unable to pass through the optic nerve to reach the central retinal artery and rescue vision loss, but may help with the associated signs of ptosis, pain and ophthalmoplegia. More common complications that we see referred to us occurring with dermal filler are largely technique related, such as overfill, Tyndall Effect and malar oedema, particularly with tear trough treatments. This area requires a good knowledge of the anatomy, assessment to exclude pre-existing oedema and septum deficiency, then if appropriate, gentle restoration, starting indirectly away from the tear troughs. Managing overfill in this area with hyaluronidase can also be a minefield, potentially resulting in further damage by the hyaluronidase to the normal anatomy and orbital septum with worsening of fat prolapse, ultimately requiring surgical correction.
KNOWLEDGE AND EDUCATION
Infection can be avoided with good aseptic technique. We routinely use the eye-safe periocular spray Purifeyes 17 which provides antimicrobial protection for patients post-treatments. Delayed hypersensitivity reactions and nodules are also rare and are usually an immune response to the filler, triggered by a systemic infection or dental intervention. A careful medical and aesthetic history will guide towards the cause and treatment.
Overall complications can be avoided with good practical anatomical knowledge. Attending a hands-on cadaveric dissection course and learning about complications prevention and management should be the first step towards a safe practice both for yourself and your patients. 18
Patients should be offered a holistic approach to facial restoration with the appropriate treatment modalities – both surgical and non-surgical – to achieve the desired outcome. If something cannot be optimally managed non-surgically or could be made worse with our treatment, then we owe it to our patients to counsel appropriately and refer for a second or surgical opinion.
REFERENCES
1. Wegrzyn M, Vogt M, Kireclioglu B, Schneider J, Kissler J. Mapping the emotional face. How individual face parts contribute to successful emotion recognition. PLoS One. 2017 May 11;12(5).
2. American Society of plastic surgeons. Plastic surgery statistics. https://www.plasticsurgery.org/documents/News/ Statistics/2020/top-five-cosmetic-plastic-surgery-procedures-2020.pdf. Accessed 10th January 2022.
3. Chopra K, Calva D, Sosin M, Tadisina KK, Banda A, De La Cruz C, Chaudhry MR, Legesse T, Drachenberg CB, Manson PN, Christy MR. A comprehensive examination of topographic thickness of skin in the human face. Aesthet Surg J. 2015 Nov;35(8):1007-13. doi: 10.1093/asj/sjv079. PMID: 26508650.
4. Bonini S, Rama P, Olzi D, et al. Neurotrophic keratitis. Eye (Lond). 2003;17:989–95
5. Zander E, Weddell G. Observations on the innervation of the cornea. J Anat. 1951;85:68–99
6. Stutman RL, Codner MA. Tear trough deformity: review of anatomy and treatment options. Aesthet Surg J. 2012 May;32(4):426-40
7. Cantisani C; Amori P; Vitiello G; Tirant M; Thuong VN; Lotti T; Matovic D; Hajzler ZP; Vojvodic A. Non surgical blepharoplasty. Dermatol Ther. 2019 Nov;32(6): 1529-8019
8. Dayan, Erez; Burns, A. Jay; Rohrich, Rod J.; Theodorou, Spero. The use of radiofrequency in aesthetic surgery.
Plastic & Reconstructive Surgery Global Open , Aug2020, Vol. 8 Issue 8, 2861-2861
9. Garg S, Vashisht KR, Sushruth PR, Saka DV. Monopolar radiofrequency for reposing drooping fat planes and facial rejuvenation: A prospective study on 30 subjects towards true antiaging. J Cosmet Dermatol. 2021;00:1– 12
10. Miedziak AI, Gottsch JD, Iliff NT. Exposure keratopathy after cosmetic CO2 laser skin resurfacing. Cornea 2000; 19: 846-848
11. Landau M; Nestor MS; de Almeida AT; Al-Niaimi F, Journal of cosmetic dermatology [J Cosmet Dermatol], ISSN:
1473-2165, 2020 Oct; Vol. 19 (10), pp. 2484-2490
12. American Society of Plastic Surgeons. Plastic Surgery Statistics. https://www.plasticsurgery.org/news/plasticsurgery-statistics. Accessed 10th January 2022
13. Murthy R, Roos JCP, Goldberg RA. Periocular hyaluronic acid fillers: applications, implications, complications. Curr Opin Ophthalmol. 2019 Sep;30(5):395-400
14. Kapoor KM, Kapoor P, Heydenrych I, Bertossi D. Vision Loss Associated with Hyaluronic Acid Fillers: A Systematic Review of Literature. Aesthetic Plast Surg. 2020 Jun;44(3):929-944
15. https://www.thepmfajournal.com/features/features/post/is-there-a-role-for-retrobulbar-hyaluronidase-inhyaluronic-acid-vascular-embolism-related-vision-loss
16. https://aestheticsjournal.com/cpd/module/retrobulbar-injections-in-filler-related-vision-loss
17. www.purifeyes.co.uk
18. www.aesthetics-course.com